
6 The lack of research in primary care settings over the past 20 years is cited as an important reason for this. According to one study, just 12 percent of pediatricians reported high self-efficacy in managing obesity, even though 39 percent believed that treatment of obesity by physicians has the potential to be effective. There is evidence that family physicians and primary care pediatricians are uncomfortable managing childhood obesity. Today, settings in which identification, prevention, and treatment of childhood obesity are practical and rational include schools, where children spend much of their time, and primary care practices, through which they receive much of their health care. Environmental changes take a long time to establish and even longer to have a substantial impact on children's health. This will probably require change in public policy that affects, for example, how certain foods are marketed to and packaged for children. Significant environmental and societal change holds the promise of reversing the problem. The widespread use of medications to treat childhood obesity is likely many years away. At best, such programs can accommodate only a fraction of the nation's obese children. Specialized centers offer effective intensive counseling programs that promote behavior modification for obese children. These include advising families to limit consumption of sweetened beverages and fast food, limit screen time, engage in physical activity for at least 60 minutes per day, and encourage family meals on most, and preferably all, days of the week.ĭespite the seriousness of childhood obesity, effective and safe prevention and treatment programs are not widely available. Many of these recommendations can be carried out by family physicians for treatment and prevention. 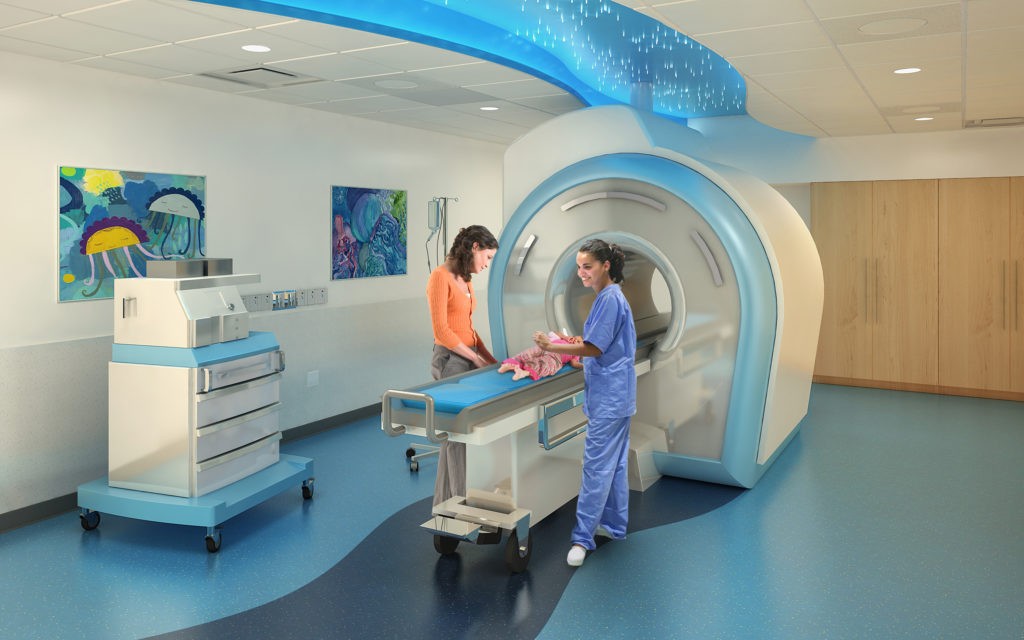
A four-stage approach to treatment of childhood obesity is recommended. Measurement of blood urea nitrogen and creatinine levels should be added in children with a body mass index above the 95th percentile. 
Those with the same body mass index and obesity-related illnesses should also have tests for alanine transaminase, aspartate transaminase, and fasting blood glucose levels. For children with a body mass index between the 85th and 94th percentiles but who have no obesity-related illnesses, a fasting lipid profile should be done. Laboratory testing recommendations depend on the degree of obesity and associated illnesses. Family physicians are urged to assess key dietary habits (e.g., consumption of sweetened beverages), physical activity habits, readiness to change lifestyle habits, and family history of obesity and obesity-related illnesses. The Expert Committee on the Assessment, Prevention, and Treatment of Child and Adolescent Overweight and Obesity recommends addressing the issue of weight with all children at least once a year. Evidence about how best to manage and prevent obesity was reviewed and incorporated into a series of reports. The American Medical Association recently convened an expert panel to address this need. Practical strategies that primary care physicians can use to tackle the problem are scarce. Childhood obesity is an increasingly serious problem 13.9 percent of children two to five years of age, 18.8 percent of children six to 11 years of age, and 17.4 percent of adolescents 12 to 19 years of age in America are obese.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
